How shrinking Medicaid reimbursement is squeezing ABA providers and what it means for families seeking autism care.
In August 2025, Nebraska slashed its Medicaid reimbursement rates for Applied Behavior Analysis services by as much as 79 percent for some billing codes. The cuts were so severe that even after the reduction, the state’s rates remain above the national average. But Nebraska is just one data point in a broader, more complicated picture reshaping the economics of autism care across the country.
A wave of Medicaid rate adjustments in the second half of 2025 has sent ripples through the ABA provider community. Some states are cutting; others are quietly raising rates. The result is a patchwork reimbursement landscape that is forcing providers to make difficult decisions about where to operate, whom to serve, and how to stay solvent while maintaining clinical quality.
The Rate Cut Landscape
Data compiled by MediRate, a healthcare reimbursement analytics firm, reveals the scope of recent changes. Greg Nersessian, President of MediRate, characterizes the current environment as “mixed”—a departure from the narrative of universal downward pressure.
“Some states that had higher rates relative to the average, or that are dealing with near-term budget issues, have brought their rates down, while other states have been increasing rates.”
Nebraska’s cuts dominate the headlines. The state reduced reimbursement for the commonly-billed 97153 code—adaptive behavior treatment by protocol, typically delivered by Registered Behavior Technicians—by 48.2 percent. Code 97154, used for group adaptive behavior treatment, fell 79.3 percent. Yet Nersessian notes that Nebraska’s rates “were so far above any other state’s that this wasn’t unexpected.”
Other states have followed with more modest reductions. Colorado cut rates across all ABA codes in October, with reductions ranging from 1.8 percent to 47.6 percent depending on the service. New York trimmed its 97153 rate by 14.3 percent. North Carolina implemented a 10 percent across-the-board cut in October, though it paused the reduction a month later and restored prior rates. Washington has announced a 2 percent cut effective January 2026.
Recent Medicaid Rate Reductions for ABA Services
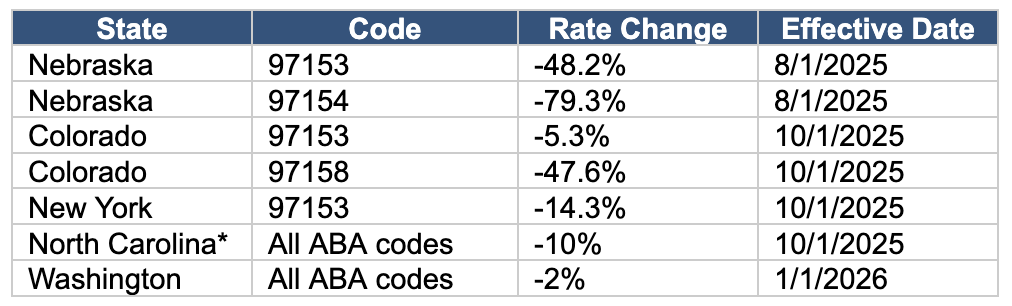
Source: MediRate. *North Carolina paused cuts in November and restored prior rates.
But rate cuts are only half the story. Texas increased all ABA codes by 11.5 percent in September. Georgia added 3 percent in July, and Utah raised rates by 1.6 percent the same month. The divergence creates strategic complexity for multi-state operators and an opportunity for those positioned in favorable markets.
The logic is circular in the best sense. Strong recruiting and training produce better clinical outcomes. Better outcomes improve client retention and generate referrals. Organic growth from satisfied families costs less to sustain than growth driven by marketing spend.
Where the Pressure Shows
For providers, rate changes rarely exist in isolation. They interact with wage pressures, staffing shortages, and the operational complexity of delivering one-on-one care to children with autism.
Thomas Spiegel, Vice President at Provident Healthcare Partners, has watched the ABA sector evolve through three distinct phases of private equity investment, as he describes them. The current phase, he says, is defined by an intensified focus on clinical quality and regional concentration—strategies that become even more critical when reimbursement tightens.
“We’re seeing pressure not initially on reimbursement, but on authorized hours per week per kid from the payers.”
When combined with rate cuts, this dual squeeze on both price and volume can devastate margins.
The pressure is already forcing some providers to make painful choices. Krista Orellana, Executive Vice President of Growth and Chief Clinical Officer at Acorn Health, says rate stagnancy and reductions have directly impacted clinical operations. “We’re having to shift away from serving Medicaid families in Tennessee and Florida, specifically, due to our inability to financially sustain, hire, and retain high-quality staff,” she explains.
When asked what gives first when margins tighten, Orellana’s answer is unequivocal: “We refuse to trade on quality and instead have had to make impossibly difficult decisions about which payers we can continue to partner with, limiting access for families.”
The staffing equation compounds the challenge. BCBAs (Board Certified Behavior Analysts) and RBTs (Registered Behavior Technicians) remain in high demand, and providers compete not just with each other but with retailers and other service industries offering comparable or better wages. In states where reimbursement has fallen behind, the math simply doesn’t work. “It’s a core issue in our states, like Florida and Tennessee, where rates are not survivable,” Orellana says.
When reimbursement falls and wage pressure persists, something has to give. Providers may reduce hours, limit caseloads, exit certain markets, or scale back the clinical infrastructure—such as supervision ratios, training programs, and outcome-tracking systems—that support quality care.
The Payer Mix Dilemma
Rate volatility is also reshaping how providers think about their business mix. Chasing high Medicaid rates has proven risky for companies that built their models around states like Nebraska or North Carolina, only to face sudden cuts.
“Having all your eggs in one basket,” Spiegel notes, “might not be the right play long term.” He advocates for diversified payer relationships—working with multiple commercial insurers alongside Medicaid—to buffer against rate shocks in any single channel.
The market differences are stark. In Texas, many ABA providers are 95 percent commercial. In states like North Carolina, Medicaid dominates the payer mix. Providers in Medicaid-heavy markets face outsize exposure to state budget decisions and rate-setting processes they cannot control.
What’s Working?
Providers navigating the rate-constrained environment are converging on a few key strategies.
Regional density over national expansion. The first wave of private equity investment in ABA saw platforms plant flags across the country, acquiring practices in California while opening centers in Virginia and Florida. That model, Spiegel says, proved “extremely difficult” to operate. Today’s successful providers focus on dominating local markets—building brand reputation, negotiating leverage with regional payers, and creating efficiencies in recruitment and supervision.
Clinical quality as a competitive asset. Outcome tracking, supervision ratios, and demonstrable clinical results are becoming table stakes for payer negotiations. Providers who can show measurable progress for the children they serve are better positioned to defend or negotiate rates. “Clinical integrity, clinical outcomes, clinical excellence,” Spiegel says, “has been super important because that will drive payer relationships and payer negotiations, which can drive higher reimbursement, which will offset a lot of the wage pressure.”
Operational efficiency without sacrificing care. Orellana says Acorn Health has focused on streamlining documentation and workflows—not as a response to margin pressure, but as a clinical imperative. “To ensure optimal outcomes, it’s paramount to us that our clinicians spend as much of their time as possible directly in client-facing work,” she explains. In practice, that means automating where possible and streamlining auditing processes.
Retention and recruitment infrastructure. Some providers have accepted that turnover among RBTs is endemic and have invested heavily in recruitment machines that can backfill departures. Others focus on career development—helping RBTs become BCBAs through in-house training programs—to build loyalty and reduce churn. Either approach requires deliberate investment that rate cuts make harder to sustain.
What It Means for Families
The ultimate concern is access. ABA therapy remains the most evidence-based intervention for autism, and demand continues to outstrip supply in most markets. Rate cuts that push providers out of Medicaid or force them to reduce capacity directly affect families—particularly those who depend on public insurance.
When providers exit a market, families feel it immediately. “When scaled providers, like Acorn, are forced to pull out of a given market due to payer rates, it substantially impacts network adequacy for families in that market,” Orellana says. The consequences are predictable: longer wait lists, reduced hours, fewer options.
Wait lists are already long in many regions. If providers respond to rate pressure by limiting Medicaid enrollment or reducing staff, those wait times will grow. Children who need early intervention may miss critical developmental windows.
The rate increase states offer a counterpoint. Texas’s 11.5 percent bump may attract providers and expand capacity. Georgia’s increase, though modest at 3 percent, signals state-level recognition that adequate reimbursement is necessary to maintain access.
The Road Ahead
The ABA sector is at an inflection point. After years of rapid growth fueled by rising autism incidence and expanding insurance mandates, providers now face a more complex operating environment where reimbursement can no longer be taken for granted.
Orellana’s outlook is clear-eyed: “I really believe that providers are going to need to continue adapting in 2026 and beyond.”
For investors and operators alike, the calculus has shifted. Geographic selection matters more. Clinical outcomes data is becoming a prerequisite, not a differentiator. And the companies that will thrive are those that can deliver quality care sustainably—even when the rates don’t cooperate.
As Nersessian’s data makes clear, the picture is not uniformly bleak. Some states are investing in autism services; others are pulling back. The challenge for providers is to build businesses resilient enough to weather the uncertainty—and for families, to find care in a system where economics increasingly shapes access.






