Key Takeaways
- Indiana’s Medicaid ABA program grew from $21 million in 2016 to $611 million in 2023, the fastest rate of growth of any state ABA program in the country.
- In January 2024, Indiana replaced an uncapped 40%-of-billed-charges model with a fixed fee schedule structured around a U-modifier credential tier.
- At April 2027 rates, Indiana will drop from the national middle tier to the lower portion of the Medicaid ABA rate range, placing its key direct treatment codes below most states currently sitting between $18 and $24 per 15-minute unit.
- The April 2026 bulletin also introduced a 1:8 RBT supervision ratio, a telehealth ban on assessment and direct treatment codes, caregiver coaching requirements in all PA requests, and expansion of 97153 billing to BCaBAs (U2) and BCBAs (U3), a code previously billable only by RBTs.
- ABA coverage is now restricted exclusively to EPSDT (members under 21) effective April 1, 2026, with a transition window through September 30, 2026 for members 21 and older who were already receiving services, after which Indiana will no longer authorize or reimburse ABA for adults.
Indiana does not make it simple to understand how Applied Behavior Analysis is paid for, or for whom. The state plan covers ABA for children, the waivers cover something analogous but distinct for adults, managed care organizations sit between providers and payment for most of the market, and a credential-tiered modifier system determines how much any given service is worth depending on who delivers it. The policy environment governing it is moving faster than almost anywhere else in the country.
The Wall Street Journal, in a March 2026 investigation into Medicaid ABA spending nationally, called Indiana “the nation’s hotbed of the booming autism therapy industry.” Indiana’s Medicaid ABA expenditures grew from $21 million in 2016 to $611 million in 2023, drawing federal scrutiny and prompting two successive administrations to intervene. The federal OIG audit of Indiana’s 2019 and 2020 ABA payments identified at least $56 million in improper claims, with every single sampled case containing at least one deficient line. More than 8,000 Hoosiers currently rely on Medicaid to pay for ABA, with more than 320 provider locations statewide and a provider count that grew 25% between 2023 and 2025 alone.
The state is now in its second major policy intervention in two years. The January 2024 fixed fee schedule replaced a 40%-of-billed-charges system. Governor Braun signed Executive Order 25-31 on February 19, 2025, establishing the ABA Working Group, which launched in May 2025 and delivered approximately 20 recommendations in November 2025. Those recommendations are now taking effect in phases through April 2027. The rate structure and policy conditions below reflect both what is in effect today and what Indiana has already announced for the next twelve months.
How Indiana Medicaid Covers ABA: EPSDT, Managed Care, and the Adult IBI Exception
Indiana covers ABA therapy for Medicaid members under 21 through the state plan, using EPSDT as the coverage vehicle. Hoosier Healthwise covers children through age 19 and pregnant women. Hoosier Care Connect covers individuals up to age 59 who are blind or disabled and not eligible for Medicare, and serves as the managed care pathway for many ABA-eligible members aged 19 and 20. Traditional Medicaid covers members outside the managed care structure. All programs require an autism spectrum disorder diagnosis and a finding of medical necessity.
Effective April 1, 2026, IHCP bulletin BT202627 restricted ABA coverage exclusively to EPSDT, formalizing the under-21 limit. Members aged 21 and older who were already receiving services have a transition window through September 30, 2026; beginning October 1, 2026, Indiana Medicaid will no longer authorize or reimburse ABA for members 21 or older.
For adults with intellectual and developmental disabilities, the state’s Home and Community-Based Services waivers, specifically the Community Integration and Habilitation waiver and the Family Supports waiver, offer Intensive Behavioral Intervention. IBI incorporates the same evidence-based techniques that underpin ABA practice but is structured and billed differently, and requires a licensed psychologist or psychiatrist at the director level.
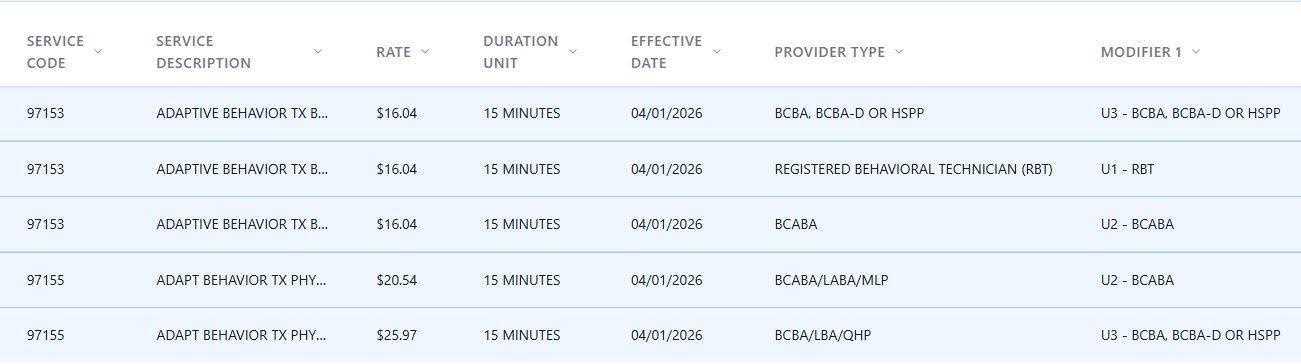
Indiana Medicaid ABA Rates by CPT Code: Current, April 2026, and April 2027
Indiana uses a three-tier modifier system to differentiate ABA reimbursement by provider credential level. The U1 modifier applies to registered behavior technicians, U2 to BCaBAs, and U3 to BCBAs and BCBA-Ds. Starting April 1, 2026, IHCP bulletin BT202627 also expanded 97153 to BCaBAs (U2) and BCBAs (U3); previously only RBTs could bill this code. All rates are billed in 15-minute units, all require prior authorization, and the state uses a maximum fee schedule methodology. The MediRate table below reflects the current post-phasedown rates effective April 1, 2026.
The table below, drawn directly from IHCP bulletin BT202627, shows the pre-reform rate for each code alongside both phases of the upcoming reductions.
|
Code |
Mod |
Pre-Apr 2026 |
Apr 1 2026 (-6%) |
Apr 1 2027 (-4%) |
Credential |
|
97151 |
U2 |
$21.87 |
$20.56 |
$19.74 |
BCaBA |
|
97151 |
U3 |
$27.63 |
$25.97 |
$24.93 |
BCBA/BCBA-D |
|
97152 |
U1 |
$17.06 |
$16.04 |
$15.39 |
RBT |
|
97153 |
U1 |
$17.06 |
$16.04 |
$15.39 |
RBT |
|
97153 |
U2 |
N/A (new) |
$16.04 |
$15.39 |
BCaBA |
|
97153 |
U3 |
N/A (new) |
$16.04 |
$15.39 |
BCBA/BCBA-D |
|
97155 |
U2 |
$21.85 |
$20.54 |
$19.72 |
BCaBA |
|
97155 |
U3 |
$27.63 |
$25.97 |
$24.93 |
BCBA/BCBA-D |
|
97156 |
U2 |
$21.87 |
$20.56 |
$19.74 |
BCaBA |
|
97156 |
U3 |
$28.23 |
$26.54 |
$25.47 |
BCBA/BCBA-D |
Prior Authorization, Supervision Ratios, Telehealth Restrictions, and Indiana’s April 2026 Policy Overhaul
IHCP bulletin BT202627 introduced several policy changes alongside the rate phasedown, all effective April 1, 2026. Understanding them together is essential because they restructure not just what Indiana pays, but how services must be delivered and documented to qualify for payment.
The supervision ratio is the most immediately operational change: the IHCP now requires a minimum of one hour of BCBA or qualifying supervising clinician oversight for every eight hours of RBT-delivered treatment. This 1:8 ratio adds a billable documentation burden and creates a structural dependency on BCBA capacity that will affect staffing models, particularly for practices with high RBT-to-BCBA ratios. The question of how many hours of ABA therapy are clinically appropriate has been central to state reform debates nationally; Indiana’s supervision requirement lands squarely in that conversation.
Telehealth restrictions represent another significant change. Starting April 1, 2026, the IHCP no longer allows 97151, 97152, 97153, 97154, or 0373T to be billed with modifier 95 (synchronous telemedicine). These codes cover assessment, protocol development, and direct treatment, which IHCP determined require in-person interaction. Supervision codes 97155 and 97156 are not on the restricted list, meaning remote oversight sessions may continue.
Caregiver coaching is now required in all ABA therapy prior authorization requests. The IHCP allows up to 18 hours over a standard six-month authorization period, with proportional adjustments for shorter authorizations. This requirement formalizes what many providers were already documenting informally but adds a distinct planned component to every authorization submission.
The April 2026 changes are the second major intervention in Indiana’s ABA reimbursement structure in two years. The federal OIG identified $56 million in improper payments during 2019 and 2020 alone, citing credentialing failures, missing evaluations, and inadequate documentation, as part of a broader audit series that has since found compliance failures in Maine and other states.
For providers evaluating Indiana’s reimbursement environment, the state presents a paradox: it is simultaneously one of the largest ABA Medicaid markets in the country and one undergoing the most aggressive reform cycle. The credential tiering system gives BCBAs a meaningful rate advantage over RBTs, and the fixed fee schedule provides more billing predictability than the prior 40% structure. But the two-phase rate phasedown, the provider moratorium, the incoming accreditation requirement, the new supervision ratio, and the telehealth restrictions collectively represent a fundamental reset of operating conditions. The broader ABA M&A market is watching Indiana closely, as the reform cycle is already influencing how acquirers model reimbursement risk in Midwest-heavy portfolios.
Frequently Asked Questions
What are Indiana’s current Medicaid reimbursement rates for ABA therapy after the April 2026 phasedown?
Effective April 1, 2026, Indiana applied a 6% reduction to all nongroup ABA codes. Post-phasedown rates per 15-minute unit: 97153 U1 (RBT treatment) at $16.04; 97155 U2 (BCaBA) at $20.54 and U3 (BCBA) at $25.97; 97151 U2 at $20.56 and U3 at $25.97; 97156 U3 at $26.54. A second 4% reduction applies to all ABA codes effective April 1, 2027, bringing 97153 U1 to $15.39 and 97155 U2 to $19.72.
Does Indiana Medicaid cover ABA therapy for adults?
As of April 1, 2026, Indiana restricts ABA coverage exclusively to EPSDT, which applies to members under 21. Members aged 21 and older receiving services have a transition window through September 30, 2026; after October 1, 2026, Indiana will no longer authorize or reimburse ABA for members 21 or older. Adults with I/DD may access Intensive Behavioral Intervention through the CIH or FSW HCBS waivers, which uses similar techniques but is structured, billed, and supervised differently.
What is Indiana’s 4,000-hour ABA lifetime cap?
Indiana’s 4,000-hour lifetime ABA service cap took effect April 1, 2026. It limits total Medicaid-covered ABA hours a child can receive over their lifetime. Children who exhaust the allocation may access up to 15 additional hours per week if continued medical necessity is documented. The cap was one of approximately 20 recommendations from Governor Braun’s ABA Working Group, whose November 2025 report addressed Indiana’s ABA spending trajectory, which peaked at $611 million in 2023.
What new supervision, telehealth, and documentation requirements took effect in Indiana in April 2026?
IHCP bulletin BT202627 introduced four major operational changes effective April 1, 2026. First, a 1:8 supervision ratio: one hour of BCBA oversight required per eight hours of RBT-delivered treatment. Second, telehealth restrictions: 97151, 97152, 97153, 97154, and 0373T may no longer be billed via telehealth. Third, caregiver coaching: required in all PA requests, up to 18 hours per six-month authorization. Fourth, 97153 expansion: BCaBAs (U2) and BCBAs (U3) may now bill this code, which was previously RBT-only.
How does Indiana’s ABA rate compare nationally, and how will it change by 2027?
Before the April 2026 phasedown, Indiana’s combined average of $21.83 for 97153 and 97155 placed it in the national middle tier. After the full two-phase reduction, 97153 U1 falls to $15.39 and 97155 U2 to $19.72 by April 2027, moving Indiana from the national middle tier toward the lower portion of the Medicaid ABA rate range, below most states currently sitting between $18 and $24 per unit. For context on how reimbursement rates affect ABA business valuations, the gap between Indiana’s trajectory and higher-rate states will become increasingly significant for operators with fixed staffing cost structures.
Why did Indiana’s Medicaid ABA spending grow so dramatically?
Indiana’s ABA spending grew from $21 million in 2016 to $611 million in 2023 because the state used a 40%-of-billed-charges model that rewarded providers for raising their billed charges. Some providers charged $600 per hour for routine sessions. The federal OIG audit found that 97 of 100 sampled cases involved services delivered by uncredentialed staff. Indiana’s provider count also grew 25% between 2023 and 2025 with no accreditation or licensure requirement limiting entry. The January 2024 fixed fee schedule and the April 2026 reforms are direct responses to this pattern.







