Key Takeaways
- A 10 percent cut was reversed. NCDHHS reduced RB-BHT rates by 10 percent on October 1, 2025 amid a Medicaid budget shortfall, then restored all 2025 rate reductions to September 30, 2025 levels after Governor Stein’s December 10, 2025 directive; updated fee schedules were posted January 5, 2026.
- A lawsuit forced the pause. Twenty-one families filed suit in October 2025 alleging discrimination; Wake County Superior Court granted a temporary restraining order and then a preliminary injunction on November 10 that blocked the ABA cut.
- Fee schedules are back to September 30, 2025 levels. Updated NC Medicaid Direct fee schedules were posted January 5, 2026, and health plans were directed to reprocess affected claims, restoring 97153 to $20.81 and 97155 to $32.22 per 15 minutes.
- Oversight legislation is advancing. House Bill 696, which cleared both chambers on second reading April 22, 2026 (House 112 to 1, Senate 48 to 1), is scheduled for third-reading votes April 28. If enacted, it would codify in-person assessment requirements, a 50 percent telehealth supervision cap, a 10 percent minimum LQASP oversight floor, and a three-tier enforcement framework for noncompliant providers.
North Carolina’s applied behavior analysis providers have spent the past six months on a policy rollercoaster. In late summer 2025, the state legislature passed a stopgap Medicaid funding bill that left the North Carolina Department of Health and Human Services about $319 million short of what it said it needed to maintain services. On October 1, NCDHHS began paying roughly 3 to 10 percent less across much of the Medicaid fee schedule. Research-based behavioral health treatment, the service category that covers ABA for children with autism, was singled out for the steepest reduction at 10 percent.
Twenty-one families filed suit in late October, arguing the state had unfairly singled out a protected class of disabled children. A Wake County judge agreed, issuing first a temporary restraining order and then a preliminary injunction on November 10 that blocked the ABA cut. A month later, Governor Josh Stein directed NCDHHS to restore Medicaid reimbursement rates to September 30, 2025 levels, a decision the Governor’s office attributed to recent court orders. Updated fee schedules were posted to the Medicaid Covered Codes and Fee Schedules Portal on January 5, 2026, restoring every code to its September 30 level.
That restoration is the status quo today. But it is not the whole story. The General Assembly and NCDHHS have spent the intervening months drafting the oversight framework for the service category the lawsuit was fought over. House Bill 696, which began as a health care practitioner transparency bill and was restructured in the conference committee substitute proposed April 21, 2026 (“Medicaid & HHS Adjust./Other Critical Needs”), cleared second reading in both chambers on April 22 (House 112 to 1, Senate 48 to 1) and is on the calendar for third-reading votes April 28. Section 3C.18 of the bill contains the most detailed set of ABA-specific requirements North Carolina has ever put into statute.
What North Carolina Medicaid pays for ABA in 2026
North Carolina covers ABA through its RB-BHT benefit, authorized under Clinical Coverage Policy 8F. The 2026 standard rate schedule, restored to September 30, 2025 levels, pays the same base rates to providers serving children under NC Medicaid Direct and those served through the Tailored Plans operated by the LME/MCOs, the regional entities that administer behavioral health and intellectual and developmental disability services. Those entities are Alliance Health, Partners Health Management, Trillium Health Resources, and Vaya Health.
At 15-minute billing units, the base ABA rates are: $30.56 for 97151 (behavior identification assessment by a physician or qualified health professional); $61.73 for 97152 (behavior identification supporting assessment by a technician); $20.81 for 97153 (adaptive behavior treatment by a technician); $11.37 for 97154 (group adaptive behavior treatment by a technician); $32.22 for 97155 (adaptive behavior treatment with protocol modification by a QHP); $23.70 for 97156 (family adaptive behavior treatment guidance); and $11.51 for 97157 (multiple-family group adaptive behavior treatment guidance).
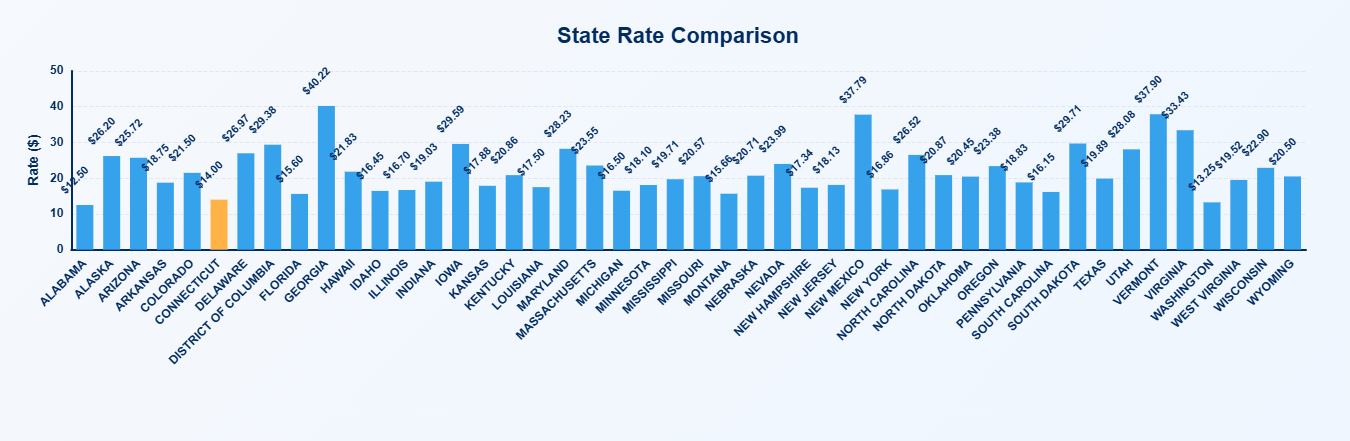
State Rate Comparison: Medicaid ABA Reimbursement (unweighted 97153 + 97155 combined average, per 15-minute unit). Source: MediRate.
On the unweighted combined average of the 97153 and 97155 procedure codes, MediRate data places North Carolina at $26.52 per 15-minute unit, in the middle of the national Medicaid ABA rate range. That figure reflects the restored post-reversal rates; the October 2025 cut would have pulled the state’s comparison figure down by roughly 10 percent before the injunction and the Governor’s December directive restored it.
Those base rates are the starting point for most providers, but the payment picture is slightly more complex. Each LME/MCO publishes its own rate schedule alongside the state fee schedule, and a handful of codes show minor specialty-level variation across entities. MediRate maintains a full, entity-by-entity Medicaid ABA rate library that providers and investors use to benchmark at a granular level, including modifier-level detail that this explainer does not attempt to replicate.
How the rate cut got reversed
The October 1 cut never took lasting hold. Twenty-one families, represented by Michael F. Easley Jr., the son of former Governor Mike Easley and a former U.S. Attorney for the Eastern District of North Carolina, filed suit in Wake County Superior Court alleging that NCDHHS had committed facial discrimination by assigning a steeper cut to a service used predominantly by children with autism. Their complaint rested on the fact that most Medicaid services received a 3 percent reduction while RB-BHT, Innovations Waiver services, 1915(i) services, and ICF programs were cut by 8 to 10 percent.
Judge Bryan Collins issued an initial temporary restraining order, and Judge Clayton Somers followed with a preliminary injunction on November 10 that blocked the ABA cut while other reductions remained in effect. NCDHHS argued in court that the cuts were proportional, pointing out that RB-BHT had received a 15 percent rate increase in January 2024 and that, per the state’s court filing, total state spending on RB-BHT was projected to climb from $199 million in fiscal year 2022-23 to $639 million in fiscal year 2025-26 even with the 10 percent reduction. That argument did not carry the day.
On December 10, 2025, Governor Stein announced a full reversal, directing NCDHHS to restore rates to September 30, 2025 levels. Provider Alliance Health, which had deferred implementation internally, confirmed it would not recoup any rate differential. Updated fee schedules were posted January 5, 2026, with instructions to health plans to reprocess claims for dates of service on or after October 1, 2025 at restored rates. The reconciliation window closed late in the first quarter of 2026. A motion by the state to dismiss the underlying lawsuit as moot was denied in March. The plaintiffs have continued to argue that without a State Plan Amendment codifying the reversal, the state could reimpose the cuts in the next budget cycle.
What HB 696 would require of ABA providers
If enacted in its current form, Section 3C.18 of House Bill 696 would direct NCDHHS to amend Clinical Coverage Policy 8F and, where necessary, seek CMS approval for a detailed set of delivery and oversight rules. The provisions target three areas: telehealth, supervision ratios, and provider enrollment.
On telehealth, the bill would bar paraprofessionals (including Registered Behavior Technicians and non-registered technicians) from delivering CCP-8F services via telehealth absent exceptions developed by the Division of Health Benefits for medical necessity or rural access. Licensed Qualified Autism Service Provider assessments would be required in person; any LQASP services involving observation and direction of a paraprofessional could be delivered by telehealth but would be capped at 50 percent of services delivered to any single Medicaid recipient. Parent and caregiver training by LQASPs would remain available by telehealth without an in-person requirement.
On supervision and ratios, the bill sets a floor and a band. At least 10 percent of all CCP-8F services provided by a paraprofessional must involve LQASP observation and direction. For any beneficiary who receives more than 200 hours of paraprofessional RB-BHT services in a six-month window, the provider would have to maintain an LQASP-to-paraprofessional hour ratio of at least 10 percent and no more than 20 percent, unless the provider can document medical necessity for exceeding 20 percent. Treatment plans exceeding 16 hours of services per week would require PHP or Department approval and would have to be reapproved monthly.
On enrollment and credentialing, the bill would formally exempt paraprofessionals from Medicaid credentialing. A 120-day grace period would allow newly hired paraprofessionals to deliver billable services while pursuing an RBT credential from the Behavior Analyst Certification Board or an ABAT credential from the Qualified Applied Behavior Analysis Credentialing Board. After 120 days, services delivered by uncredentialed paraprofessionals would not be reimbursable. Board Certified Behavior Analysts and Qualified Autism Services Practitioner Supervisors would be barred from enrolling in North Carolina Medicaid as out-of-state providers, a provision aimed at tightening the regulatory perimeter around who can bill the program.
Enforcement follows a graduated structure. A first or second occurrence of noncompliance would permit DHB to recoup payments for the noncompliant services. A third occurrence of material and systematic noncompliance would authorize DHB to suspend a provider’s eligibility to bill Medicaid for one to two years. DHB would be required to adopt rules to carry out each of these actions.
What providers should prepare for
With rates restored and HB 696 on the verge of enactment, North Carolina ABA providers face a period of dual adjustment: operational continuity under the restored fee schedule and compliance readiness for a new statutory framework. Key planning items for 2026 include mapping current telehealth delivery against the proposed paraprofessional prohibition, auditing supervision ratios to confirm the 10 to 20 percent band is achievable across high-utilization caseloads, and preparing documentation workflows for the monthly reapproval cycle on cases exceeding 16 hours per week.
The 120-day RBT credentialing grace period will be the sharpest operational change for clinics with high technician turnover. Providers with out-of-state BCBAs on staff will need to evaluate whether those clinicians should relocate, obtain North Carolina licensure, or transition off the Medicaid panel. The six-month utilization reporting requirement, aligned with the ratio compliance window, will create a new cadence of compliance documentation that DHB has not yet detailed in format or submission mechanism.
For broader context on how North Carolina’s enforcement trajectory fits the national ABA picture, see Acuity’s coverage of the federal audits exposing widespread billing failures in the ABA industry, the accountability era arriving for autism care, and the ongoing debate over ABA therapy hours and the 40-hour standard. For private equity-backed operators weighing the North Carolina market, Acuity’s analysis of the 10 largest ABA providers reshaping autism care offers useful strategic context.
Frequently Asked Questions
What are the current North Carolina Medicaid rates for ABA services in 2026?
The 2026 standard rate schedule, effective in its restored form since January 5, 2026, pays $30.56 for 97151, $61.73 for 97152, $20.81 for 97153, $11.37 for 97154, $32.22 for 97155, $23.70 for 97156, and $11.51 for 97157. All are billed in 15-minute units. These are the same rates in effect September 30, 2025 before the October rate cut was imposed and subsequently reversed.
Was the October 2025 ABA rate cut permanent?
No. NCDHHS reversed the 10 percent RB-BHT reduction, along with all other rate reductions implemented October 1, 2025, following Governor Stein’s December 10, 2025 directive. Claims submitted at the reduced rates were reprocessed by health plans at the restored rates, with reconciliation completed late in the first quarter of 2026.
What is House Bill 696 and when does it take effect?
HB 696, restructured in the conference committee substitute proposed April 21, 2026 (“Medicaid & HHS Adjust./Other Critical Needs”), cleared second reading in both chambers of the North Carolina General Assembly on April 22, 2026 and is scheduled for third-reading votes April 28. Section 3C.18 would set new requirements for ABA delivery, supervision, telehealth, and provider enrollment. Most provisions would take effect when the act becomes law, though some require NCDHHS to amend Clinical Coverage Policy 8F and, if necessary, seek CMS approval before they apply operationally.
Does HB 696 prohibit telehealth for ABA?
Not entirely. The bill would prohibit paraprofessionals from delivering services via telehealth and would require in-person assessments by Licensed Qualified Autism Service Providers. LQASPs could continue to deliver observation and direction of paraprofessionals via telehealth, but capped at 50 percent of services for any individual Medicaid recipient. Parent and caregiver training by LQASPs would remain available via telehealth with no in-person requirement. DHB may develop exceptions based on medical necessity or access concerns in rural and underserved areas.
What happens if a provider fails to meet the new supervision or credentialing requirements?
HB 696 establishes a three-tier enforcement structure. A first or second occurrence of noncompliance permits DHB to recoup payments for the noncompliant services. A third occurrence of material and systematic noncompliance authorizes DHB to suspend the provider’s Medicaid billing eligibility for one to two years.
Can out-of-state BCBAs still enroll as North Carolina Medicaid providers?
Under HB 696, no. The bill would bar Board Certified Behavior Analysts and Qualified Autism Services Practitioner Supervisors from enrolling in the North Carolina Medicaid program as out-of-state providers. This provision is effective when the act becomes law and applies to all applications for enrollment submitted on or after that date.
How do LME/MCO rates compare to NC Medicaid Direct rates for ABA?
The four LME/MCOs that administer Tailored Plan and behavioral health services (Alliance Health, Partners Health Management, Trillium Health Resources, and Vaya Health) publish entity-specific rate schedules. For the core RB-BHT codes, all four mirror the NC Medicaid Direct standard rate schedule at the base level, with limited specialty-level exceptions at some entities. For providers weighing market-by-market economics within North Carolina, entity-level detail, including modifier-specific variation, is tracked in MediRate’s Medicaid ABA rate database.
Is the lawsuit over North Carolina’s ABA cuts finished?
Not yet. Although NCDHHS argued in March 2026 that the full rate reversal made the case moot, Wake County Superior Court Judge Vince Rozier denied the state’s motion to dismiss. The plaintiffs have argued that without a State Plan Amendment codifying the reversal, the state could reimpose the cuts in a future budget cycle. The case is ongoing.







