Key Takeaways
- Fraud prosecutions are reshaping the policy environment: Federal information charges against Smart Therapy LLC and Star Autism Center LLC, both filed in the past year, allege a combined $20+ million in fraudulent EIDBI billing through cash kickbacks to families and unqualified staff.
- DHS and the Legislature have moved in parallel: A pause on new EIDBI agency enrollment took effect November 1, 2025; provisional licensure standards opened for application in January 2026 with a May 31, 2026 deadline; a 1:16 supervision ratio became effective January 1, 2026.
- HF4338 would impose billing caps across human services: The omnibus House Human Services finance bill, sponsored by Republican Representative Joe Schomacker of Luverne, includes billing limits, a codified definition of fraud, and new pre- and post-payment review requirements. Per fiscal tracking documents released by the committee, the bill in its entirety is projected to save $141.3 million in FY 2027 and $197 million in subsequent years across the full range of human services programs it covers.
- Direct-care rates land in the middle of the regional pack: Minnesota’s 97153 RBT rate of $17.95 per 15-minute unit and 97155 BCBA rate of $20.17 per 15-minute unit place the state above its Wisconsin and North Dakota neighbors but below South Dakota and Iowa, per MediRate fee schedule data.
Minnesota’s ABA-policy environment in 2026 looks little like the picture five years ago. The Early Intensive Developmental and Behavioral Intervention (EIDBI) benefit, codified at Minnesota Statutes § 256B.0949, remains the state’s primary Medicaid pathway for autism-related behavioral services. But what was once a steadily expanding program has become the focal point of a coordinated state response to fraud: federal prosecutions of EIDBI providers, new licensure standards, supervision-ratio rules, an administrative pause on new agency enrollment, and a legislative push to cap autism-services billing. Each of those tracks has been framed by state officials and bill sponsors as a program-integrity measure.
The fraud track has been the most visible. Per a December 2025 Minnesota Department of Human Services legislative report, the agency has designated EIDBI one of 14 high-risk Medicaid programs for fraud monitoring; the U.S. Attorney’s Office has confirmed it is among those currently under federal investigation. Per CBS News reporting that cites state records, all autism providers in total billed $1.6 billion across Minnesota DHS Medicaid programs from 2018 through 2025. Per a Minnesota Star Tribune analysis published in December 2025, $217.7 million in alleged fraud has been identified across state-run social services programs since September 2022, a figure that includes the Feeding Our Future child-nutrition scheme alongside Medicaid programs.
On the legislative track, EIDBI has been the subject of multiple rounds of structural change since the benefit’s creation in 2013, with major revisions enacted in 2015 and 2018 and a separate 2024 law establishing licensure for behavior analysts. The most recent set of changes is the most consequential. Laws 2023, Chapter 61 enacted a 14.99 percent rate increase that took effect January 1, 2024. Laws 2025, 1st Special Session, Chapter 9, Article 6 established a provisional EIDBI agency licensure framework, mandated a 1:16 maximum supervision ratio for behavioral aides effective January 1, 2026, and directed DHS to develop comprehensive agency licensure standards for legislative review by January 1, 2027. Effective November 1, 2025, DHS paused new EIDBI agency enrollment per a transmittal to providers; that pause remains in effect.
Provisional licensure, the supervision ratio, and the federal fraud cases
The headline reform is provisional agency licensure. Applications opened in January 2026 for agencies enrolled as MHCP providers, with a nonrefundable fee of $2,100 per application. The deadline to submit a complete application is May 31, 2026, per the DHS EIDBI Licensure Frequently Asked Questions page. Agencies that fail to apply by that date must cease operations and will be disenrolled. DHS must submit comprehensive licensure standards to the Legislature by January 1, 2027 for legislative approval before they become permanent.
The federal fraud track has run alongside the legislative one. The first federal charges arrived on September 24, 2025, when Asha Farhan Hassan, the registered owner of Smart Therapy LLC, was charged by federal information with wire fraud for her role in a $14 million EIDBI scheme. Hassan pleaded guilty on December 18, 2025 before U.S. District Judge David Doty. Per the federal filing, Smart Therapy enrolled in EIDBI in late 2019 and, between November 2019 and December 2024, defrauded the program by recruiting children from the Somali community, including children who did not have autism diagnoses, paying parents monthly cash kickbacks of $300 to $1,500 per child, and billing for services that were not delivered. Hassan was also charged in connection with the Feeding Our Future scheme, for which she received $465,000.
On the same day Hassan pleaded guilty, federal prosecutors charged Abdinajib Hassan Yussuf, the operator of Star Autism Center LLC, with wire fraud by federal information; Yussuf pleaded guilty in early March 2026. Per the filing, Yussuf and partners enrolled Star Autism in EIDBI in late 2020 and, through December 2024, recruited children from the Somali community with monthly cash kickback payments to parents, employed unqualified relatives as behavioral technicians, and obtained more than $6 million in EIDBI reimbursement from Minnesota DHS and UCare.
The 2026 billing-cap fight and where Minnesota’s rates land regionally
The 2026 legislative session has opened a new front. The House Human Services Finance and Policy Committee’s omnibus finance bill, HF4338, sponsored by Republican Representative Joe Schomacker of Luverne, would establish billing caps for disability, older adult, and behavioral health services as part of a broader package of program-integrity provisions. Per fiscal tracking documents released by the committee, the bill is projected to save $141.3 million in FY 2027 and $197 million in subsequent years across all programs it covers, though the committee has not published a separate fiscal note isolating the savings attributable to the EIDBI-specific provisions. Provisions include a codified definition of fraud in Medicaid statute, new pre- and post-payment review requirements, expanded Electronic Visit Verification, and surety-bond requirements for some provider categories.
Provider organizations have objected publicly to how those caps would apply to EIDBI. Eric Larsson, chair of the Autism Treatment Association of Minnesota, told the committee that the proposed EIDBI billing limits “come with a risk of unanticipated repercussions that can both create the risk of fraud and harm” per House Session Daily reporting on the April 15, 2026 hearing. Jay O’Neill, president of the Autism Treatment Association of Minnesota, told the same committee that “placing caps on services may prevent some children from ever reaching their full potential.” Jen Diederich, chief compliance officer at MAC Midwest, said the surety-bond and reserve requirements are “not realistic and it’s not attainable for most nonprofits and community-based providers.” The bill remained in committee at the time of this article’s publication.
Minnesota’s EIDBI fee schedule, effective January 1, 2026, pays Level I providers (BCBA, BCBA-D, and qualified equivalents) at 100 percent of the published rate and Level II providers (BCaBA and Registered Behavior Technicians) at 80 percent, per the EIDBI billing grid published by the Minnesota Department of Human Services. For 97153 (adaptive behavior treatment by protocol), the resulting RBT-tier rate is $17.95 per 15-minute unit. For 97155 (protocol modification), the BCBA-tier rate is $20.17 per 15-minute unit. Both reflect the 14.99 percent EIDBI rate increase enacted by Minnesota Laws 2023, Chapter 61, effective January 1, 2024.
The two charts below show how those rates compare to neighboring state Medicaid programs, isolating the provider tier most directly relevant to each code: RBT for 97153 (the direct-service provider who delivers the bulk of the hours billed) and BCBA for 97155 (the supervisor responsible for protocol modification).

Figure 1: 97153 RBT-tier rate per 15-minute unit, Minnesota and neighboring states. Source: MediRate.
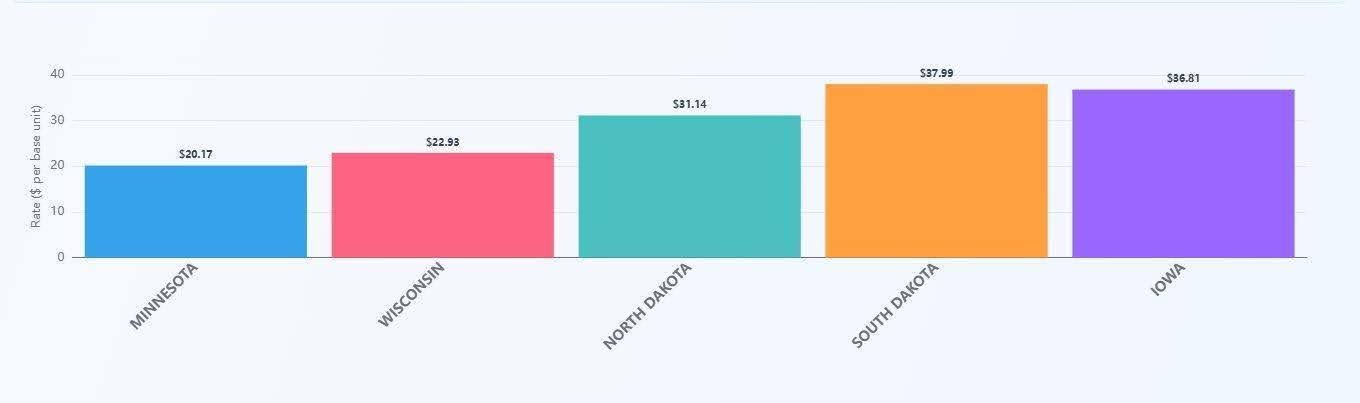
Figure 2: 97155 BCBA-tier rate per 15-minute unit, Minnesota and neighboring states. Michigan does not separately publish a 97155 rate in the comparable MediRate dataset and is therefore excluded from this chart. Source: MediRate.
On 97153, Minnesota’s $17.95 RBT rate sits in the middle of its regional pack, well above Wisconsin ($11.91) and North Dakota ($10.60) but meaningfully below South Dakota ($21.43). Iowa ($17.16) and Michigan ($16.50) sit just below Minnesota. On 97155, Minnesota’s $20.17 BCBA rate is the lowest of the five states for which MediRate publishes a comparable rate; Wisconsin pays $22.93, and the Dakotas and Iowa all clear $30. The pattern suggests that Minnesota pays comparatively well for direct-service hours but compensates supervisory time at a relatively low rate by Upper Midwest standards.
The Autism Treatment Association of Minnesota’s case against the billing limits, as Larsson laid it out in a separate exchange with Acuity following his committee testimony, rests on three connected arguments. The first is that the cross-state rate comparison can be misleading without accounting for how supervisory work is reimbursed. In Minnesota, Larsson said, clinician training, assessment, and supervision are billed transparently as separate codes, while in several neighboring states those activities are bundled into the practice-expense component of higher per-unit rates. By his analysis, that structural difference means the comparison Acuity charts above understates Minnesota’s effective gap with neighboring states: Larsson estimated that to cover the cost of supervisory activities reimbursed transparently in Minnesota but absorbed into per-unit rates elsewhere, Minnesota’s direct-service rates would need to run roughly 50 percent higher than those of states using a bundled approach. Larsson further argued that bundled-rate models can create incentives for providers who collect the higher per-unit rate without delivering the underlying supervisory work, a dynamic he said the transparent Minnesota approach is designed to prevent.
The second argument is a clinical one the association has long advocated: that meaningful ABA treatment requires high levels of individualized assessment, retraining, and clinical direction because each child’s presentation differs from the next. “Our advocacy for the right levels of authorized hours is not based on a desire to bill for exorbitant sums,” Larsson said. “It is based on our 20 years of experience with how much it takes to deliver the level of quality that families and children deserve.” In ATAM’s framing, the supervisory hours that HF4338’s billing limits would constrain are not overhead but the mechanism through which the program produces outcomes. “Meaningful treatment really depends on the high quality, accountable, continuous assessment, retraining, and monitoring that is necessary to achieve the cost-effective goals that payers should want to be achieving,” Larsson said.
The third argument follows from the first two: that capping authorized hours risks substituting a count of delivered hours for a measure of whether children make progress. The arguments above represent the trade association’s case as it heads into the HF4338 fight and reflect ATAM’s analysis of how neighboring-state rate structures, bundled-rate incentives, and the clinical economics of EIDBI interact. They are presented here as ATAM’s position and have not been independently verified against payer data from other states or evaluated against alternative analyses of the same comparison.
In national context, Minnesota’s reform pattern is in some ways more sweeping than what other states have done in 2026. Indiana’s ABA reform under Bulletin BT202627 tightened utilization through dosage and supervision ratios but did not impose licensure or pause new agency enrollment; Texas’s Medicaid ABA program has tightened audit posture but maintains a comparatively open enrollment environment. The Minnesota model layers a provisional licensure regime on top of an active federal fraud track and an enrollment pause, a combination that creates significant near-term operational uncertainty for incumbent agencies and effectively closes the door to new entrants for the duration of the pause.
For ABA operators considering Minnesota, the takeaway is that the state’s policy environment in 2026 is among the most uncertain in the country. The combination of a fraud track, an enrollment pause, a billing-cap proposal, and a new licensure regime represents the most concentrated set of structural changes any state Medicaid ABA program has faced in a single legislative cycle. On rates, the picture is mixed: Minnesota’s direct-service RBT rate for 97153 sits in the middle of the Upper Midwest pack, but its supervisory BCBA rate for 97155 is the lowest among the regional comparators MediRate tracks, which has implications for clinical-staffing economics in any operator considering market entry or expansion.
Frequently Asked Questions
What is EIDBI in Minnesota Medicaid?
EIDBI is the Early Intensive Developmental and Behavioral Intervention benefit codified at Minnesota Statutes § 256B.0949. It covers ABA and related behavioral interventions for children and youth under 21 with autism spectrum disorder or related conditions and is administered by the Minnesota Department of Human Services through Medical Assistance and MinnesotaCare.
What does Minnesota Medicaid pay for ABA in 2026?
Per the Minnesota EIDBI billing grid effective January 1, 2026, the 97153 RBT-tier rate is $17.95 per 15-minute unit (Level II providers paid at 80 percent of the Level I rate). The 97155 BCBA-tier rate is $20.17 per 15-minute unit (Level I providers at 100 percent). Rates incorporate the 14.99 percent EIDBI increase that took effect January 1, 2024 under Minnesota Laws 2023, Chapter 61.
What is the new EIDBI provisional licensure requirement?
Per Laws 2025, 1st Special Session, Chapter 9, Article 6, EIDBI agencies must apply for provisional licensure by May 31, 2026. The application fee is $2,100. DHS will submit comprehensive licensure standards to the Legislature by January 1, 2027 for approval. The 1:16 supervision ratio for behavioral aides took effect January 1, 2026.
What is HF4338?
HF4338 is the 2026 House Human Services Finance and Policy Committee omnibus bill sponsored by Republican Representative Joe Schomacker of Luverne. It would establish billing caps for disability, older adult, and behavioral health services, codify a fraud definition in Medicaid statute, and add pre- and post-payment review requirements. Per committee fiscal tracking documents, the bill in its entirety is projected to save $141.3 million in FY 2027 and $197 million in subsequent years across all programs it covers; the committee has not published a separate fiscal note isolating the EIDBI-specific provisions.
Are there active federal fraud cases involving EIDBI?
Yes. Asha Farhan Hassan of Smart Therapy LLC pleaded guilty December 18, 2025 to a $14 million EIDBI fraud scheme; Abdinajib Hassan Yussuf of Star Autism Center LLC was charged the same day and pleaded guilty in early March 2026 to a scheme that obtained more than $6 million from DHS and UCare. EIDBI is one of 14 Medicaid programs DHS designated high-risk for fraud in October 2025.







