Key Takeaways
- AHCCCS ABA spending rose from $260 million in fiscal year 2024 to $371 million in fiscal year 2025. AHCCCS previewed proposed updates to AMPM 320S through provider and family webinars on April 15 and 16, 2026.
- Arizona’s FY26 ABA fee schedule, effective October 1, 2025, uses four credential modifiers (HM, HN, HO, HP) and differentiates by place of service, with the home setting paying a premium across all codes.
- ABA is delivered through two parallel pathways: AHCCCS Complete Care MCOs for most members under 21, and the Department of Economic Security’s Division of Developmental Disabilities (DDD) for ALTCS-enrolled members with qualifying developmental conditions.
- Mercy Care terminated contracts with Centria Autism Center and Action Behavior Centers. Arizona Complete Health and UnitedHealthcare Community Plan each terminated contracts with Action Behavior Centers. Plaintiffs have estimated up to 1,000 children could lose access; AHCCCS disputes the figure.
- DDD’s HCBS Needs Tool, launched October 1, 2025 under HB2945, was paused mid-October after community concerns. An Emergency Rule now governs the transition and has been extended through October 10, 2026 while permanent rulemaking continues.
Arizona Medicaid runs Applied Behavior Analysis through two distinct delivery systems that share a fee schedule but answer to different agencies, and the policy environment around both is moving faster than it has in years. The Arizona Health Care Cost Containment System (AHCCCS) pays for ABA through its Complete Care managed care organizations for most children with autism spectrum disorder diagnoses, while the Department of Economic Security’s Division of Developmental Disabilities (DDD) serves members enrolled in the Arizona Long Term Care System (ALTCS) who meet developmental disability eligibility criteria.
Both pathways draw from the same FY26 ABA fee schedule that took effect October 1, 2025. AHCCCS ABA spending grew from approximately $260 million in fiscal year 2024 to $371 million in fiscal year 2025, per KJZZ citing AHCCCS figures, and that fiscal pressure has brought Arizona to a reform moment similar to the one playing out in Indiana.
How Arizona Medicaid Covers ABA: AHCCCS Complete Care, DDD, and the Two-Door System
For most children under 21 who qualify for Medicaid on the basis of income and have an autism spectrum disorder diagnosis, ABA is delivered through AHCCCS Complete Care. Members are enrolled with one of several contracted MCOs, including Mercy Care, Arizona Complete Health, Banner University Family Care, UnitedHealthcare Community Plan, Molina Healthcare, and Care1st, which administer authorizations and maintain provider networks within the AHCCCS geographic service areas.
For members with intellectual and developmental disabilities who qualify for ALTCS, the pathway runs through DDD. DDD contracts with its own set of MCOs and maintains a separate provider rate book for services unique to the IDD population. ABA delivered through DDD draws from the same fee schedule as AHCCCS Complete Care but is administered through DDD’s care coordination infrastructure. The practical effect for providers is that operating in Arizona means navigating two different contracting and authorization regimes for what is, clinically, the same service.
Arizona FY26 ABA Fee Schedule: Credential Tiers and the Home Premium
Arizona’s FY26 ABA fee schedule differentiates reimbursement by two variables: provider credential and place of service. Credential modifiers include HM (less than bachelor’s, used for RBT-level technician delivery), HN (BCaBA-level), HO (BCBA-level), and HP (doctoral-level services by BCBA-Ds or health service providers in psychology). Place of service is identified by standard codes, with the home setting (POS 12) paying a premium across the fee schedule relative to clinic-based delivery.
Per the AHCCCS FY26 ABA Fee Schedule effective October 1, 2025, CPT code 97153 (adaptive behavior treatment by technician) pays $17.91 per 15-minute unit at the HM tier, rising with credential level and home setting. CPT code 97155 (adaptive behavior treatment by a professional) pays $25.05 at HN and rises through HO and HP tiers, again with home-setting premiums. Granular rate detail by modifier and place of service is available through MediRate’s state Medicaid ABA database.
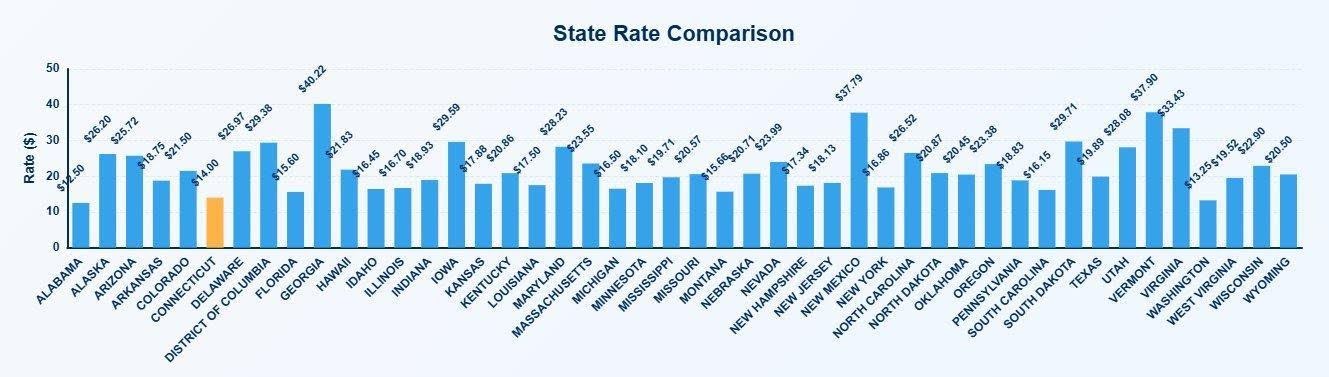
On the unweighted combined average of the 97153 and 97155 procedure codes, MediRate data places Arizona at $25.72 per 15-minute unit, in the upper-middle of the national Medicaid ABA rate range. The national spread runs from around $12.50 at the low end to above $40 in states like Georgia and New Mexico.
The Contract Terminations, the Lawsuits, and the AHCCCS Reform Package
Between October 2025 and early 2026, three of Arizona’s AHCCCS MCOs acted against two of the state’s largest ABA provider organizations. Mercy Care notified Centria Autism Center on October 17, 2025 that it was terminating its contract, following a 25 percent rate reduction effective October 1 and an earlier 15 percent reduction in July. Mercy Care subsequently terminated its contract with Action Behavior Centers as well. Arizona Complete Health and UnitedHealthcare Community Plan each separately terminated contracts with Action Behavior Centers. Contract terminations took full effect March 5, 2026.
Per Centria’s public network-status statement on March 11, 2026, the company remains contracted with Banner University Family Care, UnitedHealthcare Community Plan, Arizona Complete Health, Molina Healthcare, and Care1st, meaning the contract change applied specifically to Mercy Care. Centria’s suit, filed December 15, 2025 in Maricopa County Superior Court against Mercy Care, AHCCCS, and DDD, also alleges that Hopebridge received a termination notice from Mercy Care, though Hopebridge has not publicly confirmed its contracting status.
On February 6, 2026, eleven families filed a separate class action lawsuit in Maricopa County Superior Court against AHCCCS, alleging that the agency’s approval of the insurers’ network changes violated the federal Medicaid Act’s access requirements, the Americans with Disabilities Act, the Developmental Disabilities Act, the Arizonans with Disabilities Act, and the Arizona Constitution. Plaintiffs estimated that up to 1,000 children could lose access to their established ABA providers. AHCCCS disputed that figure in court filings, arguing that Mercy Care’s remaining network has capacity for more than 1,000 members. Families held a rally at the State Capitol on March 5, the day contract terminations took effect.
The disputes, which echo the broader spread of MCO-driven rate cuts across state Medicaid programs, have drawn attention to the extent to which private equity-backed national ABA providers depend on MCO contract continuity. Centria, Action Behavior Centers, and Hopebridge are all backed by private equity firms and are among the largest autism therapy organizations in the country, a dynamic captured in recent research on private equity’s expansion into the ABA market.
Against that backdrop, AHCCCS has signaled a policy response. The agency told KJZZ in February 2026 that it planned to publish significant ABA reforms for public comment in the coming weeks and that the package would include requirements for all providers to meet licensure and fingerprint clearance requirements as a condition of AHCCCS provider registration. On April 3, 2026, AHCCCS announced two informational webinars to preview proposed updates to AMPM 320S, the section of the AHCCCS Medical Policy Manual that governs ABA services. The provider session was held April 15 and the family session April 16. Substantive detail of the proposed AMPM 320S revisions has not yet been posted to the agency’s public comment portal as of publication.
HB2945, the Paused HCBS Needs Tool, and the Emergency Rule
HB2945, signed by Governor Hobbs in April 2025, required DDD to implement a strengthened person-centered assessment tool. AHCCCS launched the HCBS Needs Tool (HNT) on October 1, 2025, but paused it mid-October after significant pushback from the DDD community. Governor Hobbs directed AHCCCS to revise the tool and create an exception pathway, the Extraordinary Care Review (ECR) process, for members whose needs exceed what the HNT would assess.
An Emergency Rule took effect October 15, 2025. Health plans, including DDD and the EPD health plans, returned to prior assessment tools while revisions proceed. AHCCCS received more than 4,600 public comments on draft policies and has been pursuing regular rulemaking based on the Emergency Rule. The Emergency Rule will be renewed for an additional 180 days through October 10, 2026 while the permanent rule is finalized. Hobbs’s office has cited projected Contract Year 2026 savings of $133.2 million in total fund dollars and $47.4 million in Arizona General Fund dollars from the reform package, though those projections reflect the original design before the implementation pause.
What Arizona ABA Providers Should Watch in 2026
Three dynamics warrant close attention across the remainder of the year. First is the formal publication of the AMPM 320S redline and any associated fee schedule or policy changes, which will be subject to a public comment period per AHCCCS’s standard process. Second is the progress of the Centria and class action lawsuits, which could shape the scope of MCO discretion over network composition and rate negotiations going forward. Third is the evolution of DDD rulemaking following the HNT pause, and how the permanent rule reconciles fiscal sustainability with community access concerns.
Arizona’s combined average rate of $25.72 places the state in a comparatively strong position relative to many other Medicaid ABA markets, but the operational volatility of the last twelve months has meaningfully altered the calculus for providers evaluating market participation. As evolving CPT billing restrictions and supervision standards continue to reshape state Medicaid ABA programs nationally, Arizona’s next moves will likely influence how other states approach similar cost and access pressures.
Frequently Asked Questions
What is the current Arizona Medicaid ABA reimbursement rate?
Under the AHCCCS FY26 ABA fee schedule effective October 1, 2025, CPT code 97153 (technician-delivered adaptive behavior treatment) pays $17.91 per 15-minute unit at the HM (RBT-level) tier, with higher rates at the HN, HO, and HP credential tiers and additional premiums in the home setting (POS 12). CPT code 97155 (professional-delivered treatment) starts at $25.05 and rises with credential and place of service. All rates require prior authorization through the appropriate MCO or DDD contractor. MediRate maintains the granular modifier- and place-of-service detail.
Does Arizona Medicaid cover ABA therapy for adults?
ABA coverage under AHCCCS is primarily structured around members under 21 through the Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefit. Adult members with qualifying developmental disabilities may access behavioral services through DDD under ALTCS, though the service mix and delivery model differ from ABA as traditionally delivered to children.
What is AMPM 320S and what changes is AHCCCS proposing?
AMPM 320S is the section of the AHCCCS Medical Policy Manual that establishes requirements for Behavior Analysis Service delivery and treatment under Arizona Medicaid. AHCCCS held informational webinars on April 15 and 16, 2026, to preview proposed updates. The agency has stated publicly that the broader reform package will include licensure and fingerprint clearance requirements for providers as a condition of AHCCCS provider registration. The complete proposed policy text and formal public comment period have not yet been posted as of publication.
Which MCOs terminated contracts with which ABA providers?
Mercy Care terminated contracts with both Centria Autism Center and Action Behavior Centers. Arizona Complete Health and UnitedHealthcare Community Plan each terminated contracts with Action Behavior Centers. Per Centria’s March 11, 2026 public statement, the company remains contracted with Banner University Family Care, UnitedHealthcare Community Plan, Arizona Complete Health, Molina Healthcare, and Care1st. Centria’s December 2025 lawsuit alleges Hopebridge also received a termination notice from Mercy Care, though Hopebridge has not publicly confirmed its contracting status. Terminations took full effect March 5, 2026.
What happened to the DDD HCBS Needs Tool?
AHCCCS launched the HCBS Needs Tool (HNT) on October 1, 2025, pursuant to HB2945. It was paused mid-October 2025 after community pushback. An Emergency Rule took effect October 15, 2025, creating the Extraordinary Care Review (ECR) process, and health plans returned to prior assessment tools while AHCCCS revised the package based on more than 4,600 public comments. The Emergency Rule has been extended through October 10, 2026 while permanent rulemaking continues.
How does Arizona’s ABA reimbursement compare to other states?
On the unweighted combined average of CPT codes 97153 and 97155, Arizona’s $25.72 per 15-minute unit places the state in the upper-middle of the national Medicaid ABA rate range, per MediRate data. The national spread runs from around $12.50 at the low end to above $40 in states like Georgia and New Mexico. State-to-state comparisons are complicated by differences in credential tier structures, place-of-service differentials, and managed care versus fee-for-service administration.
Sources: MediRate; Arizona Health Care Cost Containment System (AHCCCS); AHCCCS FY26 ABA Fee Schedule effective 10/01/2025; Arizona Department of Economic Security Division of Developmental Disabilities; KJZZ; Arizona Mirror; Arizona Capitol Times; Axios Phoenix; Maricopa County Superior Court filings; Centria Autism network status statement (March 11, 2026).







