Key Takeaways
- New York was the 49th state to implement Medicaid coverage of Applied Behavior Analysis, with the benefit becoming billable in 2021 and widely used only beginning in 2023.
- Effective April 1, 2026, the Medicaid reimbursement rate for CPT code 97153 (technician-delivered adaptive behavior treatment) dropped to $14.45 per 15-minute unit, completing a 25% reduction phased in two 12.5% tranches authorized by the FY 2025-2026 enacted budget.
- A joint NYSABA and CASP survey found that 74% of Medicaid ABA providers indicated they would leave the program if the second rate reduction took effect.
- Governor Hochul’s FY 2026-2027 Executive Budget proposed a Centers of Excellence designation framework alongside additional cuts totaling $28.5 million over two years, which provider associations and U.S. Representative Ritchie Torres publicly opposed.
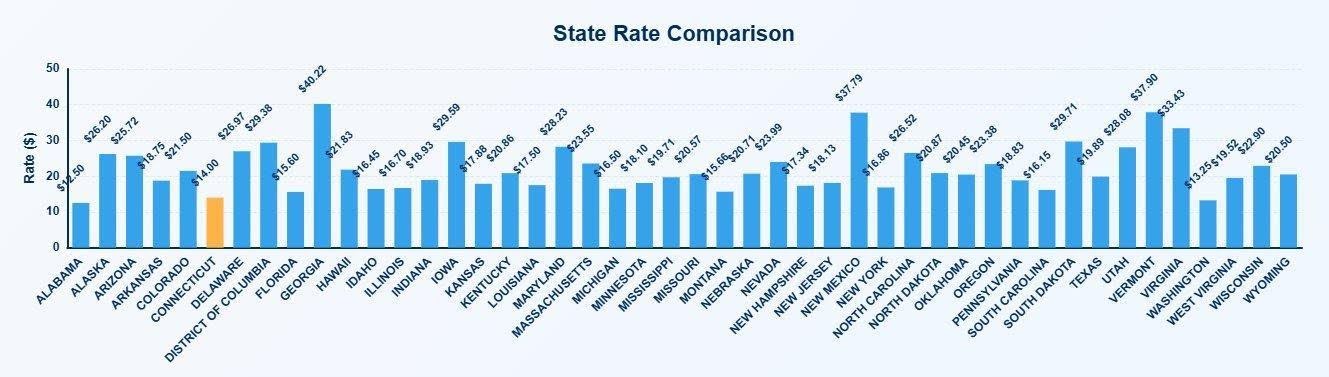
- New York’s unweighted combined average of $16.86 per 15-minute unit places it among the lowest-paying Medicaid ABA programs in the country.
New York came to Medicaid coverage of Applied Behavior Analysis later than almost any other state, and the benefit has had a short and uneven life. ABA became billable under New York State Medicaid in 2021, following more than a decade of advocacy after the state legislature first mandated commercial insurance coverage in 2012. Implementation challenges, including a limited pool of enrolled Licensed Behavior Analysts (LBAs), meant the benefit was not widely used until 2023. New York was the 49th state to implement Medicaid ABA coverage.
That brief window of expansion is now contracting. The enacted state budget for FY 2025-2026 authorized a 25% reduction in the Medicaid reimbursement rate for technician-delivered ABA, phased in across two 12.5% tranches. The first took effect October 1, 2025, reducing the rate for CPT code 97153 from $19.26 to $16.85 per 15-minute unit. The second, effective April 1, 2026, brought the rate down to $14.45. Provider associations and advocates have warned that the combined reduction will force a meaningful share of the state’s Medicaid ABA providers out of the program entirely. New York’s approach has focused on reimbursement reductions, a pending Centers of Excellence designation, and broader budgetary pressures stemming from federal Medicaid changes under the One Big Beautiful Bill Act.
How New York Medicaid Covers ABA: EPSDT, MMC Carve-In, and the LBA Credential
New York State Medicaid covers ABA therapy for members under 21 with a diagnosis of autism spectrum disorder as defined by DSM-5 and/or Rett Syndrome, accessed through the Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefit. Referrals must come from a NYS-licensed and Medicaid-enrolled physician, psychologist, psychiatric nurse practitioner, pediatric nurse practitioner, or physician assistant. ABA services were carved into the Medicaid Managed Care (MMC) benefit package effective January 1, 2023. Providers delivering ABA to MMC members must contract with the member’s MMC plan, while FFS claims are submitted through eMedNY. ABA is not reimbursable when delivered in a school setting.
Credentialing is governed at both the state and federal level. Individuals providing ABA services under NYS Medicaid must hold a Licensed Behavior Analyst (LBA) or Certified Behavior Analyst Assistant (CBAA) credential issued by the New York State Education Department. CBAAs cannot bill the NYS Medicaid FFS program directly. LBAs enrolled in the Medicaid FFS program can bill for services rendered by CBAAs under their supervision. Unlicensed individuals, referred to in New York statute as Behavior Technicians or paraprofessionals, may deliver services under LBA supervision but cannot independently bill Medicaid.
New York Medicaid ABA Fee Schedule: The April 2026 Rate Structure
Effective April 1, 2026, the NYS Medicaid fee schedule pays $14.45 per 15-minute unit for CPT code 97153 and $19.26 per unit for the remaining individual codes (97151, 97152, 97155, and 97156). Group codes 97154, 97157, and 97158 pay $3.31 per unit per member. Rates are uniform across the state and do not vary by geography or place of service. The 97153 reduction was implemented pursuant to the FY 2025-2026 enacted state budget, and the August 2025 NYS Medicaid Update framed the change as an adjustment to reimbursement methodology intended to ensure providers of ABA services are compensated equitably for their training and experience. MediRate maintains the full state-by-state comparison.
On the unweighted combined average of CPT codes 97153 and 97155, MediRate data places New York at $16.86 per 15-minute unit, well below the national midpoint and among the lowest-paying Medicaid ABA programs in the country. The full national spread runs from around $12.50 at the low end to above $40 in states like Georgia and New Mexico. Neighboring and comparable states pay meaningfully more: New Jersey sits at $18.10, Connecticut at $14.00, and Massachusetts at $23.55.
The Second Cut, the 74% Exit Survey, and the FY 2026-2027 Executive Budget
The 25% rate reduction reflected in the FY 2025-2026 budget was framed by the Hochul administration as an adjustment to reimbursement methodology distinguishing compensation for licensed professionals from compensation for unlicensed technicians. Provider associations characterized it differently. The New York State Association for Behavior Analysis testified before the state legislature in February 2026 opposing an additional round of reductions proposed in the Governor’s FY 2026-2027 Executive Budget, which included $9.6 million in cuts for the 2025-2026 fiscal year and $19 million for 2026-2027, totaling $28.5 million over two years.
In its February 2026 testimony, NYSABA reported that a joint survey it conducted with the Council of Autism Service Providers found that 74% of responding Medicaid ABA providers indicated they would leave the program if the second rate cut were implemented. The association wrote that most of its members serving Medicaid children had been able to weather the first October 2025 reduction, but that some providers had already suspended Medicaid services and that those remaining in the network were, in the association’s language, bracing themselves for April 1, 2026.
The Executive Budget also proposed a Centers of Excellence designation for ABA providers, which the Hochul administration described as a framework to ensure that ABA treatments are clear and appropriate. NYSABA raised concerns that the designation could create additional administrative barriers for families and providers, including potential delays for new referrals if pre-authorization from a Center of Excellence were required before services could begin. Qualifying criteria, the designation’s role in the referral and treatment pathway, and implementation timelines had not been made public as of the legislature’s budget hearings.
U.S. Representative Ritchie Torres publicly opposed the proposed cuts in a March 2025 letter to Governor Hochul, arguing that reducing reimbursement for Registered Behavior Technicians would drive workers out of the field. The broader spread of Medicaid rate pressures on ABA providers across states, including Georgia’s CareSource 20% rate cut and MassHealth supervision-based recoupments, has amplified concern among provider organizations that the cumulative effect of state-level reductions could reshape which providers remain viable in Medicaid markets.
Federal Medicaid Pressure and the Children’s Consolidated Waiver
New York’s ABA policy decisions are unfolding against a backdrop of significant federal Medicaid change. The One Big Beautiful Bill Act, signed in July 2025, imposed new eligibility and funding provisions that, per Governor Hochul’s public statements, will create a multi-billion-dollar impact on New York’s healthcare system. State officials have signaled that 300,000 to 450,000 New Yorkers may lose Essential Plan coverage in July 2026, with broader Medicaid effects to follow.
Beyond the ABA fee schedule, New York delivers a range of behavioral health and habilitation services to children through the Children’s Consolidated Waiver, a 1915(c) Home and Community-Based Services waiver. The April 1, 2026 Children’s HCBS fee schedule includes targeted inflationary increases of 2.6% for specified services and 1.7% for other waiver services, and consolidates Day Habilitation into Community Habilitation. ABA itself is not a Children’s Waiver service and is billed separately under EPSDT.
What New York ABA Providers Should Watch in 2026
Three dynamics warrant close attention across the remainder of 2026. First is the operational effect of the April 1 rate reduction on provider participation, which will become visible through network churn, authorization volumes, and any public reporting by MMC plans on ABA access. Second is the final disposition of the Centers of Excellence framework and any associated regulations or guidance. Third is the outcome of state budget negotiations and whether the legislature modifies or reverses elements of the proposed FY 2026-2027 reductions. Providers operating in multiple states may also track how clinical ownership requirements evolve, with Illinois’s Section 150 CPOM law now requiring BCBA ownership of ABA practices by January 2027 and similar questions surfacing in New York policy conversations.
The gap between New York’s rates and those of neighboring states also creates potential dynamics around provider relocation and multi-state operations, especially for organizations backed by private equity investors who are closely tracking Medicaid rate trajectories across state markets. As New York approaches the five-year anniversary of its Medicaid ABA benefit, the trajectory from implementation to rate reduction has compressed the arc that most state ABA benefits followed over a much longer period.
Frequently Asked Questions
What is the current New York Medicaid ABA reimbursement rate?
Effective April 1, 2026, the NYS Medicaid fee schedule pays $14.45 per 15-minute unit for CPT code 97153 (technician-delivered adaptive behavior treatment) and $19.26 per unit for 97151, 97152, 97155, and 97156. Group codes 97154, 97157, and 97158 pay $3.31 per unit per member. The 97153 rate represents a 25% reduction from the pre-October 2025 rate of $19.26, phased in across two 12.5% tranches.
When did New York Medicaid start covering ABA?
ABA became billable under New York State Medicaid in 2021, more than nine years after the state legislature mandated commercial insurance coverage in 2012. Implementation barriers, including a limited pool of Medicaid-enrolled Licensed Behavior Analysts, meant the benefit was not widely utilized until 2023. ABA was carved into the Medicaid Managed Care benefit package effective January 1, 2023. New York was the 49th state to implement Medicaid ABA coverage.
Why did New York cut Medicaid ABA rates?
The 25% rate reduction for CPT code 97153 was authorized in the FY 2025-2026 enacted state budget and framed by the Hochul administration as an adjustment to reimbursement methodology, intended to differentiate compensation based on provider training and experience. The rate change applies only to 97153, which is the code used when services are delivered by technicians rather than licensed behavior analysts. The administration has separately proposed additional reductions and a Centers of Excellence designation framework in the FY 2026-2027 Executive Budget.
What is the NYSABA survey finding about providers leaving Medicaid?
In February 2026 testimony before the state legislature, NYSABA reported that a joint survey it conducted with the Council of Autism Service Providers found that 74% of responding Medicaid ABA providers indicated they would leave the program if the second 12.5% rate reduction took effect on April 1, 2026. The association warned that providers who had weathered the first reduction were nevertheless reconsidering continued Medicaid participation.
What is the proposed Centers of Excellence designation?
Governor Hochul’s FY 2026-2027 Executive Budget proposed a Centers of Excellence designation for ABA providers, which the administration described as a framework to ensure ABA treatments are clear and appropriate. Qualifying criteria, implementation timelines, and the designation’s role in the referral and treatment pathway had not been publicly detailed as of the legislature’s budget hearings. NYSABA has raised concerns that the framework could create administrative barriers and delays for families seeking access to ABA services through Medicaid.
How does New York’s ABA rate compare to other states?
On the unweighted combined average of CPT codes 97153 and 97155, New York’s $16.86 per 15-minute unit places the state among the lowest-paying Medicaid ABA programs in the country, per MediRate data. The national spread runs from around $12.50 at the low end to above $40 in states like Georgia and New Mexico. New York pays less than most neighboring states, including New Jersey ($18.10) and Massachusetts ($23.55).
Sources: MediRate; NYS Department of Health; eMedNY NYS Medicaid Applied Behavior Analysis Services Fee Schedule effective 4/1/2026; NYS Medicaid Update, August 2025 Volume 41 Number 8; New York State Association for Behavior Analysis testimony (February 10, 2026); Council of Autism Service Providers; FY 2025-2026 and FY 2026-2027 NYS Executive Budget documents.







