Key Takeaways
- Veterans and first responders with PTSD have limited effective treatment options: standard medication management produces symptom improvement in roughly 11 to 13 percent of patients, compared to the 60 percent reductions JLC Services reports across its eTMS programs.
- State governments are functioning as de facto payers: veterans, first responders, and law enforcement officers in JLC’s state-funded programs pay nothing for treatment because states underwrite the cost, with Ohio’s program codified under Ohio Revised Code 5119.20.
- JLC Services operates more than 20 eTMS clinics across seven states under a hybrid model: state-funded programs run in Ohio, Florida, Missouri, and Massachusetts, with private insurance clinics in Virginia, North Carolina, and Georgia. The state contracts require quarterly outcomes reporting to legislatures.
- Outcomes data across 3,200 patients shows 60% reductions in validated anxiety, depression, and PTSD assessment scores: the figure has held steady regardless of patient demographics or geography as the program has scaled.
- Sleep improvement appears to be the primary mechanism: eTMS recalibrates disrupted brainwave frequencies using each patient’s individual EEG data, and patients consistently report meaningful sleep gains within the first several days of treatment.
- Wave Neuroscience, the company powering the eTMS program, received FDA Breakthrough Device Designation for its MeRT system (Magnetic EEG-guided Resonance Therapy, the personalized TMS protocol that underlies the state programs) for PTSD in December 2024 and has completed its pivotal randomized controlled trial for PTSD; clearance anticipated in the next six months could open commercial insurance reimbursement and allow the model to expand beyond state contracts.
Joe Charles was not looking for a career in brain health. He had spent decades writing software for Ford, Motorola, and Procter and Gamble, running a technology services firm in Ohio, when a former business partner, a retired Navy SEAL who had gone on to win a seat in the Ohio Senate, called him about a treatment the special operations community had been using for both performance optimization and acute neurological recovery.
Charles sat in on a phone call. He could not spell most of what the doctors were discussing. He flew to Indiana to spend three days at a pair of autism clinics using the technology. He called his partner on the drive home.
“There’s something here,” he told him.
That conversation, roughly six or seven years ago, set in motion what is now JLC Services, Inc., the Ohio-based company Charles leads as President. JLC operates as the program administrator and clinic operator for eTMS programs powered by Wave Neuroscience, the Newport Beach-based company whose EEG-guided TMS platform, called Magnetic EEG-guided Resonance Therapy (MeRT), underlies all of the treatments. MeRT is a personalized application of transcranial magnetic stimulation: rather than applying a fixed stimulation protocol to every patient, the system begins with a quantitative EEG to map each person’s individual brainwave patterns, then generates a treatment protocol calibrated to that person’s optimal pulse frequency. JLC today runs more than 20 clinics across seven states under a hybrid model, combining state-funded programs for veterans, first responders, and law enforcement officers with private insurance clinics that operate outside the state-contract framework. Charles described eTMS as directly addressing the behavioral health sector’s unmet demand for non-pharmacological treatments that produce measurable outcomes. JLC is the operator that has been building that case in state capitals, one data dashboard at a time.
The technology is the same underlying platform developed by Wave Neuroscience: a process that begins with a quantitative electroencephalogram to map a patient’s individual brainwave patterns, then uses that data to generate a personalized transcranial magnetic stimulation protocol. Where standard TMS applies stimulation at a fixed frequency and location for all patients, eTMS targets each person’s optimal pulse frequency, the rate at which a healthy brain should be firing, and uses gentle magnetic pulses to help the brain synchronize back to it.
“It’s all about communication in the brain,” Charles said. “When a traumatic event, a car accident, whatever it is, disrupts that communication, the brain starts firing at the wrong frequency. We map out your optimal pulse frequency and gently pulse that signal into the neurons. Gradually the brain starts going: this is where I should be firing.”
How eTMS Improves Sleep in Veterans and First Responders
The most consistent thing patients report in the first days of treatment is sleep. Charles describes this as the primary mechanism behind the outcomes data JLC publishes monthly. Beyond sleep, patients in the programs consistently describe reductions in irritability, restlessness, and cravings, alongside functional improvements in focus, patience, energy, and mood regulation, the constellation of day-to-day effects that the validated assessment scales translate into clinical scores.
Treatment consists of 15-minute sessions delivered Monday through Friday over 20 days. Three EEGs are collected, on day zero, day ten, and day twenty, tracking changes in brainwave activity across the course. Patients remain enrolled in the program for a full year after treatment ends. Every clinic employs peer mentors, veterans, retired police officers, or firefighters, whose role is to create an environment where patients feel comfortable enough to engage.
“Veterans love talking to veterans,” Charles said. “Police officers like talking to other police officers. They don’t like talking to doctors about what’s really going on. But they’ll talk to another veteran all day long.”
The peer mentor model has also shaped how JLC approaches access in ways that go beyond clinical design. The Scotty Brauer Foundation, a nonprofit affiliated with JLC, covers indirect costs including housing and travel for patients who need assistance getting to treatment, ensuring the program stays fully free for participants. The approach addresses a barrier that behavioral health programs broadly struggle to solve: patients do not complete treatment if the logistics of getting there become an obstacle.
In Miami, fire departments bring entire crews to the clinic in a truck so one person can receive treatment while the others remain on call. In Cleveland, squad cars sit in the parking lot outside JLC’s clinic while officers in full uniform get a 15-minute session before heading back on duty.
eTMS Outcomes Data: 60% Reductions Across 3,200 Patients
JLC publishes de-identified outcomes data monthly. Across 3,200 patients treated to date, the organization is seeing 60% reductions in validated anxiety, depression, and PTSD assessment scores. The figure has not declined as the sample has grown, which Charles, who approaches the program as a software developer rather than a clinician, treats as the most important signal in the dataset. The broader challenge of collecting and acting on outcomes data in behavioral health has been a persistent industry problem; JLC’s monthly publishing cadence and legislator-facing dashboards represent a model that other state-funded programs have not replicated.
“When we first published, we had an N of 30, and we had 60% reductions in PTSD, anxiety, and depression,” he said. “I kept thinking the more we published and the higher the N got, the numbers would start going down. I’ve got 3,200 patients in our database and I still have a 62% reduction in anxiety and PTSD. The brain is the brain. Geography doesn’t matter. Demographics don’t matter.”
The database Charles references is not a static report. JLC maintains a dashboard that aggregates patient counts, validated assessment results, and EEG data across its state-funded initiative.
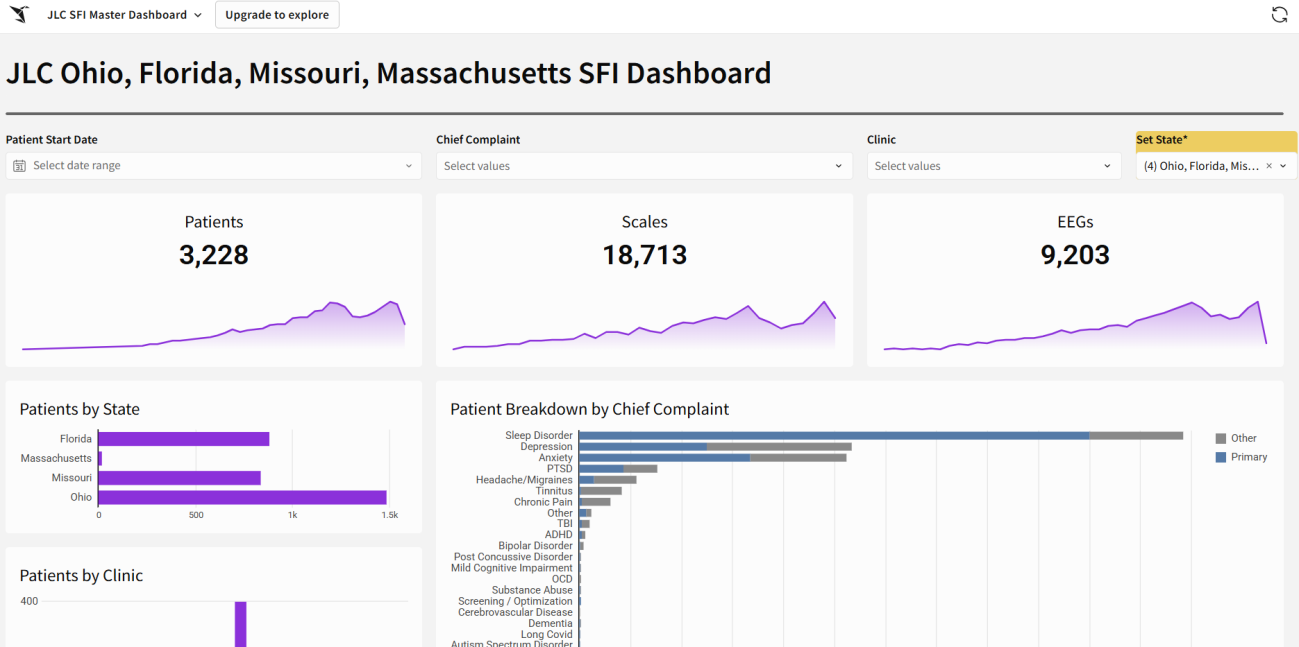
Figure 1: JLC’s state-funded initiative dashboard aggregates patient volume, validated assessments, and EEG collection across Ohio, Florida, Missouri, and Massachusetts. As of the most recent update, the dashboard reflects 3,228 patients, 18,713 assessment scales, and 9,203 EEGs. Sleep disorder, depression, and anxiety are the three most common chief complaints at intake.
Underneath the aggregate view, the program reports scale-by-scale reductions across eight validated clinical instruments, a level of granularity unusual for publicly funded behavioral health programs.
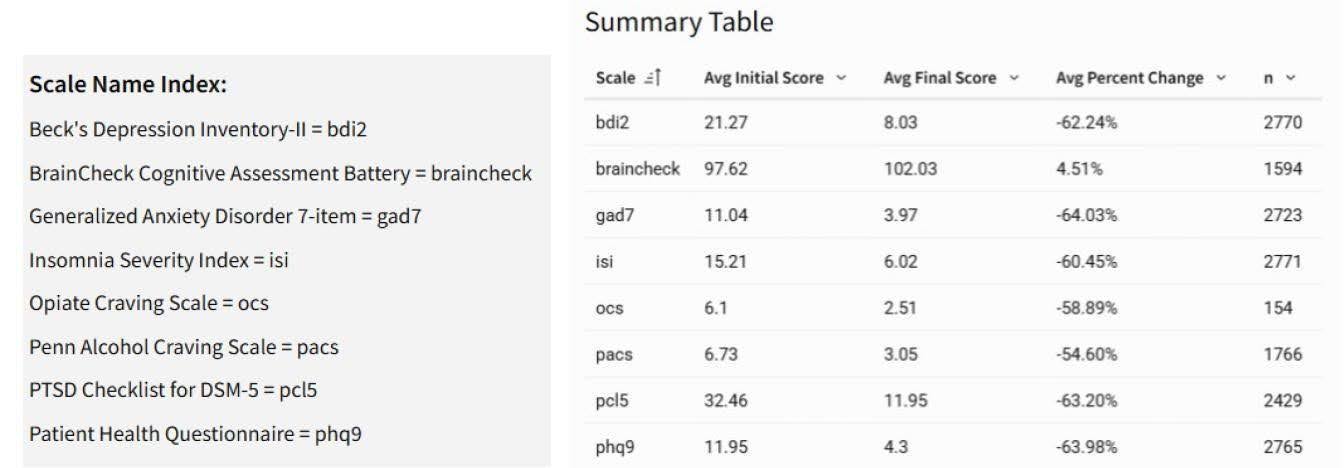
Figure 2: Average initial and final scores across the eight validated assessments JLC uses in its state-funded initiative. Seven of the eight show reductions in symptom scores, with the PCL-5 (PTSD Checklist for DSM-5) at 63.2 percent, the PHQ-9 (Patient Health Questionnaire) at 64.0 percent, and the GAD-7 (Generalized Anxiety Disorder 7-item) at 64.0 percent. BrainCheck, the cognitive assessment battery, is the outlier in that it measures improvement directly rather than symptom reduction, so a positive change is the expected direction.
Ohio alone has seen more than 1,400 patients treated. The state program began because legislators, initially skeptical, agreed to fund a small pilot after Charles brought veterans to the statehouse to speak for themselves. The results of that pilot led to sustained funding. The state-funded model has since been replicated in Florida, Missouri, and, as of February 2026, Massachusetts, where JLC has opened a clinic in Somerville and is awaiting further legislative action following completion of a pilot project. JLC also operates private insurance-based clinics in Virginia, North Carolina, and Georgia, which do not rely on state budget allocations. Massachusetts has become an increasingly active state for behavioral health program funding decisions; its legislature is simultaneously weighing a June 2026 cliff for school-based mental health funding that has put other program sponsors on notice.
Roughly two years ago, JLC began placing the technology in two inpatient addiction treatment facilities serving the general public. Among 177 patients tracked for drug of choice, Charles says the program is showing a 70% reduction in fentanyl cravings and a 40% reduction in methamphetamine cravings. Nursing staff report a measurable difference in the quality of counseling sessions for patients receiving the treatment alongside standard addiction programming. The addiction treatment industry is under its own structural pressure: as Acuity has reported, in-network migration is reshaping how SUD providers are valued and how care is delivered, making non-pharmacological adjuncts with hard outcome numbers increasingly attractive to operators and payers alike.
The state of Ohio is now pursuing a research project with JLC to answer two questions its budget office considers essential: how long the treatment’s effects last, and whether patients who complete the program demonstrate improved employment outcomes. The latter framing reflects how state systems have come to evaluate the intervention.
“If you can take someone who was addicted to fentanyl and couldn’t work, clean them up, and they find a job, you go from being a tax burden to a taxpayer,” Charles said. “That’s huge for any state.”
FDA Clearance for MeRT: What It Means for State eTMS Programs
JLC has operated entirely within state contract frameworks throughout its existence, with licensed physicians directing clinical use of the technology for conditions within the scope of current FDA clearances, while also allowing physicians to use clinical judgment in cases that may be considered “off label” use, a common and legally recognized practice in medicine. Wave Neuroscience, whose platform powers the programs, received FDA Breakthrough Device Designation for its MeRT system for PTSD in December 2024 and has completed its pivotal randomized controlled trial. FDA Breakthrough Device Designation accelerates the development and review process for technologies that demonstrate potential to provide more effective treatment for serious or life-threatening conditions; as Acuity has covered, FDA clearance carries significant commercial implications for behavioral health technology companies.
Clearance for PTSD would not limit the range of conditions physicians choose to treat with the technology, since physician-directed use for conditions beyond a specific FDA clearance is standard medical practice, but it would create a new pathway for reimbursement. Charles is direct about what that means.
“If we get clearance for PTSD, insurance can cover a certain percentage of that population,” he said. “We get more people through. There are more opportunities for both sides.”
For now, the state contract model functions as its own form of payer coverage: legislatures fund the programs, treatment is free to qualifying veterans and first responders, and the data generated flows back to the agencies that funded it. It is a structure that echoes what value-based care investors have been pursuing more broadly in behavioral health, with outcomes data serving as the currency of continued funding rather than claims volume. Charles is already talking to legislators in additional states. The pitch has gotten considerably easier.
“We now just go to states and show them our data, and they tell us they haven’t seen a program getting these kinds of reductions,” he said. “Some states jump in immediately. Some want a small pilot first. But after the pilot, the data speaks for itself.”







